We like to believe we’re prepared.
Healthcare systems run disaster drills.
We build emergency operations plans.
We check boxes that say “ready.”
But the question isn’t whether we have a plan.
The question is: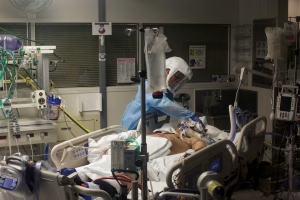


 Can we function when everything is strained at the same time?
Can we function when everything is strained at the same time?
Because that’s what large-scale conflict does.
What Large-Scale Conflict Actually Looks Like
It doesn’t arrive as a single event.
It doesn’t look like a contained mass casualty incident.
It looks like:
- A surge that doesn’t stop
- Supply chains that don’t recover
- Staffing that doesn’t rebound
- Patients who are sicker, longer
We’ve already seen pieces of this.
COVID-19 showed us what happens when:
- ICU capacity is exceeded
- Staff burnout compounds daily
- Resources become finite
Now layer that with:
- Infrastructure disruption
- Regional instability
- Prolonged operational demand
This isn’t theoretical.
This is the trajectory of modern crises.
The Illusion of Preparedness
Most systems are built for short-term disruption.
- A few hours of chaos
- A single incident
- A defined surge
However, large-scale conflict creates something different:
👉 Sustained system degradation
And that’s where things start to break.
Not because people don’t care. Not because teams aren’t skilled, but because:
- Systems rely on resupply
- Staffing models assume recovery time
- Protocols assume stability will return
When those assumptions fail, the system doesn’t flex, it fractures.
Where the System is Most Vulnerable
From both frontline and operational experience, the gaps are predictable:
1. Staffing
We are already operating lean.
There is no surge workforce waiting on standby.
When demand increases:
- Fatigue sets in quickly
- Decision-making degrades
- Retention becomes the next crisis
2. Supplies
We depend on just-in-time delivery.
That works, until it doesn’t.
IV fluids, blood products, medications, PPE-all become pressure points when disruption is prolonged.
3. Throughput
Emergency departments are already full.
Now imagine:
- No inpatient beds
- Delayed discharges
- Continuous incoming volume
There is no decompression point.
4. Communication
In stable systems, communication is structured.
In crisis:
- Information is incomplete
- Guidance changes rapidly
- Teams rely on trust, not perfect clarity
If that trust isn’t built beforehand, communication breaks down fast.
This isn’t about Fear-it’s about Accuracy
This conversation matters because preparedness is often framed as reassurance.
But real preparedness requires discomfort.
It requires asking:
- What happens if help doesn’t come?
- What happens if this lasts longer than expected?
- What happens if we have to operate differently than we ever have before?
Those are not worst-case questions. They are planning questions.
What Healthcare Professionals can do Right Now
You don’t need to control the system to improve your readiness.
Start here:
✔ Know your role in chaos
Not your job description, your function when things break down.
✔ Build comfort with imperfection
Crisis care is not textbook care.
It is good enough, fast enough, to save lives.
✔ Strengthen your team
The system doesn’t hold under pressure, people do.
✔ Understand your environment
Where are your bottlenecks?
What disappears first?
What becomes critical?
✔ Prepare mentally
Because the biggest shift isn’t operational. It’s psychological.
Final Thought
Large-scale crises don’t create weaknesses in healthcare systems.
They expose the ones that were already there.
The goal isn’t to predict the next conflict.
The goal is to be ready to function when the system is no longer working the way we expect it to, and that starts with honesty.
If you’re in healthcare, this isn’t someone else’s responsibility.
It’s ours.